Breast Implant Infections are rare, but when they happen, prompt medical care is required. The most common source for a Breast Implant Infection is the skin or glands of the breast. The breasts contain a collection of glands that open on the skin’s surface at the nipple. Bacteria are normally found on the surface of the skin and inside the breast ducts. These bacteria do more good than harm. They protect us from other, more dangerous bacteria and other potential invaders.
You might think that infection rates would be lower for Breast Reconstruction, since a mastectomy removes the breast glands and any bacteria inside; however, Breast Implant Infections occur twice as often for Breast Reconstruction patients compared to Cosmetic Breast Augmentation patients.
Many precautions are taken before, during and after your Breast Augmentation to prevent the otherwise helpful bacteria from getting under the skin and causing an infection. Even under the best of circumstances, however, surgical site infections can occur.
The most common timing for a Breast Implant infection is a few days after surgery. Normally, your post operative pain decreases daily. If your pain begins to progressively gets worse, this is not expected, and you should call promptly for an evaluation. The cardinal signs of infection are pain, redness, swelling and fever, but you may not have all the signs. Breast Implant Infections can also occur well after surgery, but this is less likely.
This page will give you information about Breast Implant Infections. It can complement, but it cannot replace actual medical care and advice. If you have a Breast Implant Infection, the sooner your treatment is started the better. If you think you have an infection, call your Plastic Surgeon and let them know what you are experiencing. If you cannot contact your Plastic Surgeon, contact your primary medical doctor, or go to your local Urgent Care Clinic / Emergency Department for prompt treatment.
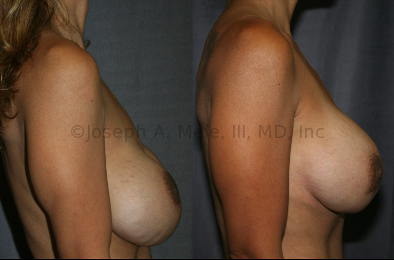
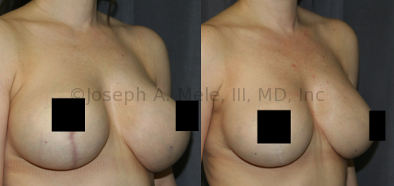
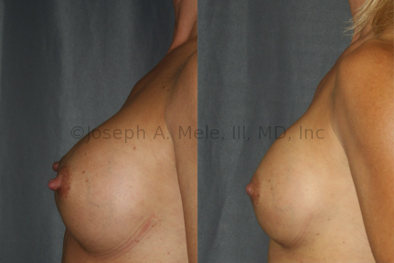
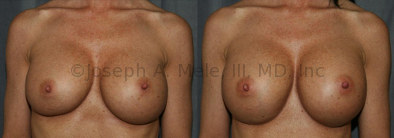
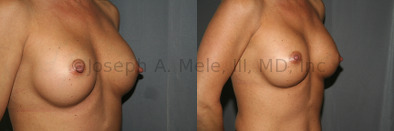
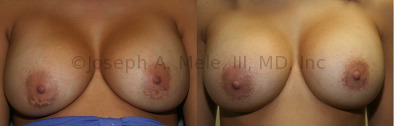
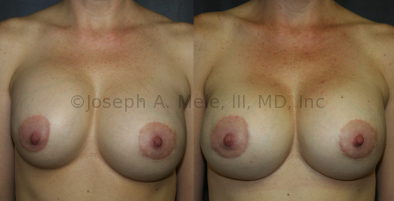
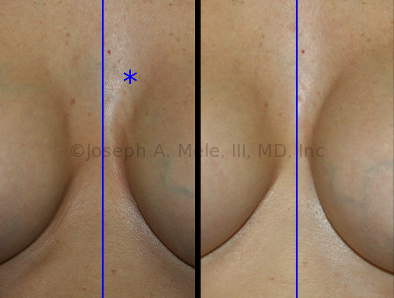
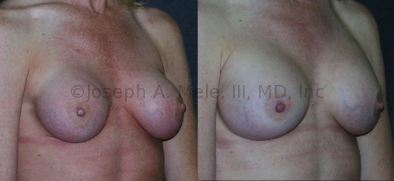
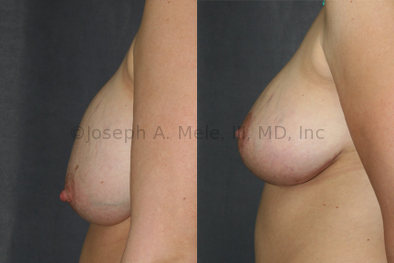
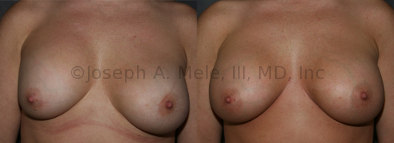
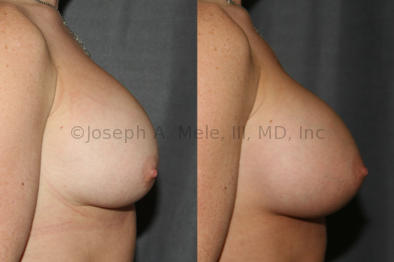
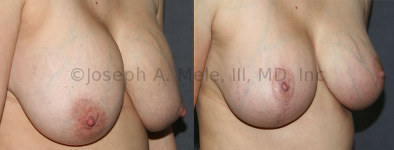
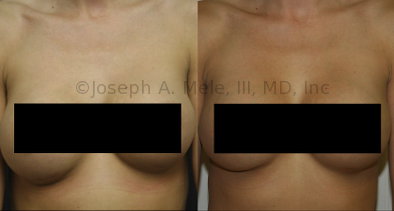
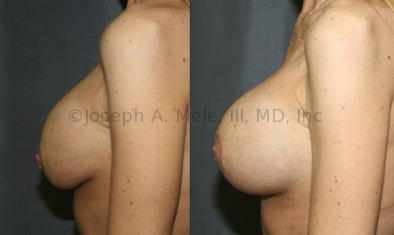
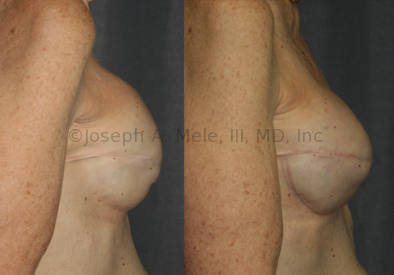
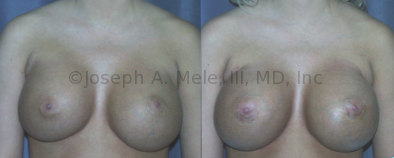
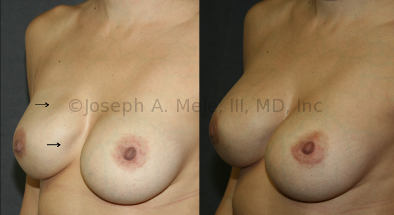
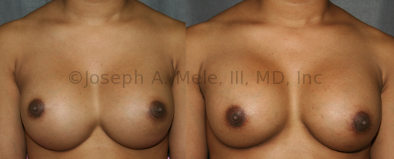
Breast Implant Revision Before and After Photos

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
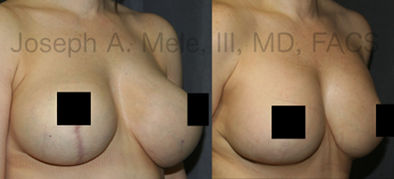
Breast Implant Revision Surgery for Infection/Exposure
Revision surgery for infection usually requires multiple surgical procedures, which may need to be scheduled months apart to prevent recurrence. Because of this, multiple precautions are taken during every Breast Augmentation and Breast Augmentation Revision surgery. Below, some of the precautions and operative treatments are reviewed. For a specific patient these may or may not apply, so be certain to check with an experienced Board Certified Plastic Surgeon in your area for guidance.
Breast Implant Infection Prevention
A rare complication of Breast Augmentation is Breast Implant Infection. Breast implant infections occur most commonly during the first few days after surgery, but can occur years later. The rate of Breast Implant Infection in the first year after Breast Augmentation is about 1%. This is the same incidence seen with any “clean” surgery. The risk of infection increases dramatically if you have a preexisting infection at the time of surgery. This seems obvious when the preexisting infection is on the breast; however, the risk is increased even with infections remote from the breasts, like urinary tract infections and upper respiratory infections.
If you have a cold or infection, all elective (non-emergency) surgery, including Breast Enhancement, should be postponed until you are well. It is not worth increasing your risk of an surgical site infection. As the saying goes, “An ounce of prevention is worth a pound of cure.” While rescheduling surgery may be inconvenient, not rescheduling can be disastrous.
All medications you take, prescription or otherwise, should be discussed with your Plastic Surgeon, prior to your procedure. In some cases, the pre-operative use of antibiotics increases your risk of an operative infection. Some medications, such as steroids and arthritis medications, may inhibit your body’s ability to fight infection. For Breast Reconstruction patients in particular, chemotherapy should be started after you are healed, or surgery should be delayed until after you have finished chemotherapy to avoid healing problems and an increased risk of infection. Medications that thin the blood increase your risk of bleeding, and may also increase your risk of infection. However, prior to changing or stopping any medication, you should first discuss it with the doctor prescribing the medication and your Plastic Surgeon.
Breast Implant Infection Prevention during Breast Augmentation
The proper planning, surgical setting and recovery is important. Many safeguards are taken during your Breast Implant Surgery to minimize your risk of infection. Dr. Mele performs Breast Augmentation only in accredited surgical facilities. This assures us of a clean and safe operative environment, that is independently inspected for quality.
Intravenous antibiotics are given just prior to the start of surgery. A warming blanket is used to prevent you from getting cold during surgery. Cold patients get more infections. The skin is throughly cleansed to reduce the bacteria on the skin, and large barrier drapes are placed over you, to prevent contamination from any areas not surgically prepared. Care is taken during surgery to minimize bleeding, as this also reduces the risk of infection.
When it is time to place the implants, a new pair of sterile surgical gloves are used to handle the implants. The implants are inspected and placed into an antibiotic solution. The pockets, where the Breast Implants are placed, are also irrigated with the antibiotic solution. The Breast Implants are then inserted, and the incision closed. The goal is to place the Breast Implants with minimal touching and minimal time exposed to the air. Implants placed behind the muscle have a better blood supply around, less breast tissue touching them and a lower incidence of infection. This is especially when the Breast Implants are used for Breast Reconstruction.
Acellular Dermal Matrix (ADM) is associated with a higher incidence of seroma formation and infection. ADMs like AlloDerm, Allomax, Collamend, FlexHD, Periguard, Strattice, Surgimend, Surgisis, Tutopatch, Veritas, XenMatrix are used sometimes for Breast Reconstruction and less frequently for certain types of Breast Implant Revision surgery. They can provide additional soft tissue coverage and support that may not be otherwise available, and may be necessary to correct specific problems. When they are not needed, however, there is a lower risk of infection.
Breast Implant Infection Prevention after Breast Augmentation
Once the implants are in place, your body will protect them by forming a Breast Implant Capsule. In addition to holding the Breast Implants in place, the capsule provides additional circulation that serves as a barrier to infection. If a Breast Implant Infection does develop, the Breast Implant Capsule’s blood supply helps to deliver antibiotics to the area around the Breast Implants.
Some Plastic Surgeons will keep you on antibiotics for a short time after surgery, and some even recommend prophylactic antibiotics before dental work. Large studies do not support the routine use of antibiotics, except in the peri-operative time period.
Breast Implant Infection Treatment
If a Breast Implant is infected, antibiotics should be started without delay. Depending on the situation, oral antibiotics may be given, or for more severe infections intravenous antibiotics will be started. Most post-operative Breast Augmentation infections are superficial, not deep around the Breast Implant. In these cases the signs of infection should resolve quickly, in a few days.
When the infection is deep, around the Breast Implant, or if the infection is associated with a collection of fluid or Breast Implant Exposure, surgical intervention may be necessary. When the infection will not resolve, or the implant becomes exposed, the best treatment is the temporary removal of the Breast Implant. This allows the chest to heal and time for the inflammation to resolve. While this may seem drastic, sometimes this is the only way to get the infection to clear.
After healing fully, the Breast Implant can be safely replaced. This is normally delayed for several months to prevent a second infection, and to allow the chest wall to recover. Trying to replace the Breast Implant too soon after an infection leads to increased bleeding, difficultly getting the implant in the proper position and a higher incidence of recurrent infection.